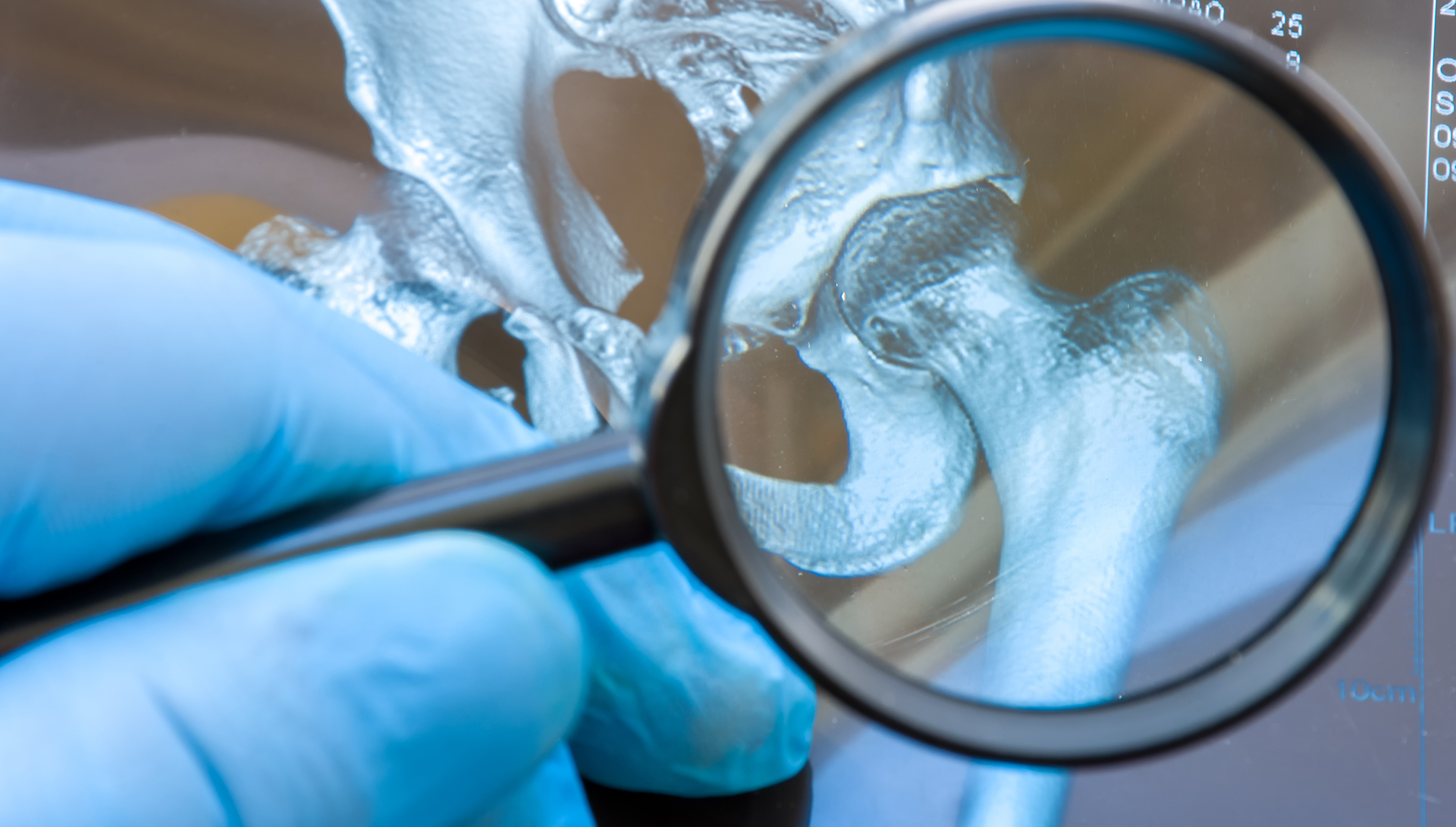
I left the doctor’s office feeling dazed, sad and full of questions. Sitting behind the wheel of my car, holding the brochures the rheumatologist had given me, I began to process what I’d been told. On one of the brochures, a pair of elderly hands were crossed on a lap, weird glowing red heat spheres emanating from the joints of the knuckles and wrists. “RA, rheumatoid arthritis, an auto-immune condition,” it was titled.
Auto-immune? What’s that? Can we fix it? Does it go away? Is there medicine? How long to I need to take it? Will it get worse? Why did I get this? As I started my car and buckled my seatbelt, I didn’t realize I was embarking on a difficult but enlightening journey that continues to this day.
RA Treatments
I learned there is no cure for auto-immune conditions, but treatments can lessen symptoms and relieve pain. Current medications include:2
- non-steroidal anti-inflammatory drugs (commonly known as NSAIDS)
- immune suppressing medications like methotrexate, (a medication used in larger doses, for chemotherapy)
- other disease modifying anti-rheumatic drugs (DMARDs)
There are more targeted antibody-blocking therapies in a newer class of drugs called biologics that use an array of modified proteins to inhibit various and particular inflammatory signals that contribute to disease activity.
Pharmaceutical therapies offer benefits and risks. An immune system that is acting inappropriately can cause harm, and suppressing it can give rise to opportunistic infections like tuberculosis and fungal infections. Immune suppression has also been associated with the occurrence of heart disease, and certain cancers, such as lymphoma.
Wondering what to do, I talked with people who use those medications. They seemed to be doing fine, with no problems. My general practitioner confided that his wife has RA and was getting infusions of a popular biologic. She was doing well.
I put off deciding on a course of rheumatoid arthritis therapy for almost two years.
I wrestled with the idea of being dependent on a pharmaceutical therapy for the rest of my life, along with the attendant risks, balanced with the knowledge I was accumulating progressively degenerative effects of RA over time. I had faith that there would be another way; those drug therapies would be there if I changed my mind.
My Information Quest
I researched online RA communities for success stories or warnings of alternative therapies, and found a link to the anti-inflammatory food pyramid.3 It is the creation of Dr. Andrew Weil, an M.D. and a naturalist, with a history in the public health community.
The idea of anti-inflammatory food hadn’t occurred to me. I didn’t feel like my diet was particularly bad. It was a normal American diet: processed meals and snacks, meats, vegetables, bread, potatoes, pasta, milk and cheeses, soft drinks, candy and cookies. I didn’t make the connection between what I was eating and the severity of my RA symptoms. More on that in a minute.
The RA “Flare”
Others with RA wrote of experiencing a “flare,” a sudden onset of severe symptoms and pain. I didn’t understand the concept of a flare because my pain and symptoms were severe all the time.
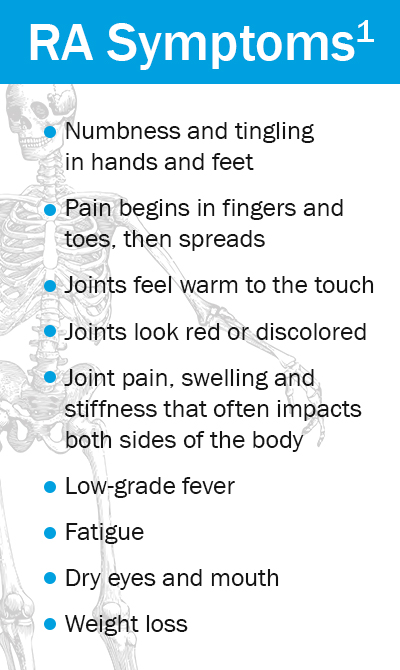
The most visible RA symptoms are the effects of the body’s joints. Typically the joint problems are bilateral: occurring on both sides of the body simultaneously, something that distinguishes rheumatoid arthritis from osteoarthritis (OA). While OA is not an auto-immune condition, it also causes wear and tear on joints, but sometimes just unilaterally.
RA’s reddened, swollen and painful joints, and the limping and stiffness associated with the disease, are easy to observe. But unseen inside the body, the attack of antibodies rages against healthy tissue. Every organ is at risk. Inflammation is the culprit and must be dampened.
The Impact of Inflammation on RA
Reading Dr. Weil’s articles I learned that all foods can be separated into inflammatory, anti-inflammatory and inflammatory neutral foods. I had been eating all types of inflammatory foods, worsening the severity of my symptoms. Who knew? Convenient, processed frozen dinners, packaged cold cuts and boxed instant meals are laden with unhealthy fats, sodium, and additives and preservatives, all contributing to inflammation.
On the vanguard of immunology there is developing knowledge that the microbiome in the gut is actually the seat of the immune system. We have more microorganisms than human cells. More than half of what makes you, you, is not you. Gut bacteria are part of signaling pathways that “teach” the body proper immune response and help it to avoid chronic disease.
A healthy gut is a diverse gut.4 Non-beneficial bacteria can proliferate and dominate, overshadowing the positive effect of the diverse collection of beneficial microorganisms. Studies have pointed to diets high in refined carbs and sugars, laden with preservatives and additives as favoring a less diverse collection of harmful bacteria that contribute to things like “leaky gut” syndrome.5 This damage and improper signaling from harmful bacteria affect inflammation, the brain and the level of pain.
Foods that Soothe My Inflammation
In addition to cultivating a healthy gut, I discovered that certain molecules in food can exert a positive reaction on the human body. Tart cherries contain anthocyanins and phenols that, for me, has reduced pain and inflammation.6 Double blind, peer reviewed studies have shown cherries to be clinically equivalent to NSAID drugs like naproxen. NSAIDs have potential side effects, such as stroke and other cardiovascular and gastrointestinal problems.7 And in a taste test, cherries win, hands down!
Turmeric is another potent medicinal food I learned about and integrated. Turmeric is a tropical plant, in the same plant family as ginger. The amazing molecule in turmeric is called curcumin.8 It’s what gives turmeric its characteristic yellow hue. (Interestingly, the anthocyanins in cherries are the chemical that makes them red. Resveratrol is a potent antioxidant. It is what gives watermelons, tomatoes, red grapefruit, strawberries and red wine grapes their colors. It’s as though nature created medicines with bright signs, in order to be noticed.)
No to Sugar and Processed Foods
I began to make some changes. You won’t find sugar in my kitchen. There is no pancake mix, there is no frozen tortellini. Gallons of cow milk are a thing of the past. Hemp milk and other plant based milks are preferred. Butter is out, extra virgin olive oil and coconut oil is in. No other vegetable oils with the exception of coconut oil are used. Nothing containing the ubiquitous corn syrup (it’s not digestible and stored as fat around your liver until your liver is the size of a king salmon.) That means no popular brands of ketchup, no packaged snacks, no candies, cookies, frozen pizza, red meat or other processed foods. Pasta and refined carbs are kept to a minimum. If pasta is eaten, the anti-inflammatory approach would be to prepare it al dente, not more than perhaps once a week.
Yes to Fruits and Nuts
Fruits have become a big part of my anti-inflammatory diet. I shoot for a wide variety of colors and lots of berries. By eating from all the colors of the spectrum you get a broad array of the beneficial antioxidant molecules that berries provide. Every fruit has its own benefits and contributes to overall health and the level of inflammation in the body.
Nuts like pistachios and walnuts are anti-inflammatory. Pistachios are also a delicious and healthy treatment for E.D. in men, and in some countries a course of pistachios is recommended before trying the little blue pill! (Peanuts are not actually nuts; they’re legumes. My research shows they are inflammatory, partly due to the saturated fats).
Meat and Potatoes…and Fish
I avoid red meats. They have high levels of saturated fats, often contain hormones or antibiotics, and are also high in histamines, which contribute to inflammation. A less inflammatory choice of protein would be white meat chicken, or cold water fish. Cold water fishes like salmon, tuna, cod, pollock, mackerel and sardines are high in omega-3 fatty acids, shown to have antioxidant properties that fight inflammation and contribute to cardiac health.
Starchy, white potatoes are best substituted with sweet potatoes, which are anti-inflammatory. Corn is inflammatory and I avoid it. An anti-inflammatory diet is not designed for weight loss, but some people have shed pounds once they’ve adopted it.
Supplements
I also take supplements. Vitamin C is easy to derive from fresh fruits and vegetables. People with RA may be deficient in vitamin D. I avoid dairy and supplement with 5,000 to 15,000 IU of vitamin D3 for anti-inflammatory action and immune support. I take Zinc and folic acid. I also supplement with fish oil; the omega-3 oils are key in lowering inflammation.
Note: before you change your diet and use supplements, it’s a good idea to talk to your primary care physician or rheumatologist.
The Future
So far, 12 years into the course of this progressive and degenerative auto-immune disease, my condition has improved. While I still visit my rheumatologist twice a year, for bloodwork and consultation, I have still not gone on a permanent pharmaceutical therapy. For a few years I used prescription NSAIDs, over-the-counter pain relievers and prescribed narcotic pain relievers. With a few exceptions, it’s been years since I’ve needed to take a pill of any kind to deal with inflammation.
I’m not cured. I have bad days. I get flares and often they are associated with periodic lapses in my diet. I have suffered some permanent joint damage and that process continues. I don’t know what the future holds, but who does? I do feel empowered by taking ownership of my health and working changes into my lifestyle that pay off in more good days than bad.
RA propelled me on a healthcare journey of discovery that continues to this day. I feel like I’m better off for it and I’m grateful for this opportunity to share part of my story.
1Mayo Clinic, “Rheumatoid Arthritis”
2Ibid
3WebMD, “Andrew Weil’s Anti-inflammatory Diet”
4WebMD, “How Your Gut Health Affects Your Whole Body”
5Harvard Medical Publishing, “Leaky Gut: What Is It?”
6Life Extension Foundation, “Anti-inflammatory Properties of Tart Cherry”
7Cleveland Clinic, “Non-steroidal Anti-inflammatory Drugs (NSAIDs)”
8U.S. National Library of Medicine, NIH, “Curcumin: a Review of Its Effects on Human Health”
MORE RESOURCES
Healthline, “A Certain Type of N95 Mask May Do More Harm Than Good”
U.S. Food and Drug Administration, “N95 Respirators, Surgical Masks and Face Masks”